Your Money or Your Life
Carolyn Morris
In a country with supposedly universal coverage, some of the most vulnerable must pay cash for health care. It costs them their livelihoods — and sometimes their lives
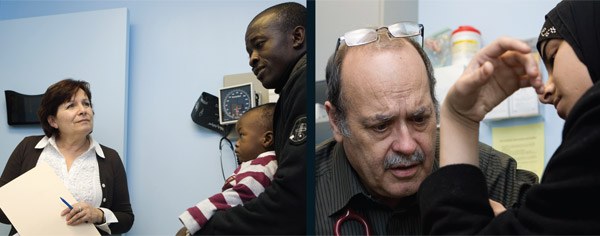
Nurse Jennifer D'Andrade and Dr. Paul Caulford consult with patients at the volunteer clinic in Scarborough. Photos by Arantxa Cedillo.
Dr. Paul Caulford will never forget what happened to Patricia. An 18-year-old girl from Grenada, she had an athletic build, black skin, and black hair cropped at her ears. She had come to Toronto at the age of 15 and her father had applied to sponsor her, but the family split up and Patricia’s father let the sponsorship drop. She had no immigration status, no health-care insurance, and peculiar blood. Patricia had sickle-cell anemia, a condition that’s particularly common among people of African descent. In places where malaria is prevalent, those with sickle-cell anemia were evolutionarily preferred because their blood was too hostile for malaria to survive. But it can also be deadly. When Patricia’s blood cells don’t get enough oxygen, they morph from their regular sphere shape into what look like crescent moons and clog up her smallest blood vessels.
Caulford explains how Patricia had gone to a clinic in extreme pain and the doctor had sent her to the emergency room. She was having a sickle-cell crisis. At the hospital, she was told she’d have to pay at least $350 before seeing a doctor because she didn’t have health insurance. But she didn’t have the money either. Patricia decided to stay anyway, and sat in the emergency room, writhing in pain, until she fell unconscious. Only then was she admitted and given an IV. She spent days in the hospital recovering and racked up a bill in the thousands.
Patricia’s was one of the many stories shared over meals by a group that included Caulford, the chief of family medicine at the Scarborough Hospital at that time, Yasmin Vali, the hospital’s director of community and patient relations, and Jennifer D’Andrade and Cathy Tersigni, two public health nurses working in shelters and with the homeless. Their dinner meetings turned into planning sessions and resulted in Canada’s only volunteer clinic exclusively — and openly — serving the uninsured.
Citizenship and Immigration Canada plans to accept as many as 265,000 new immigrants in 2009, most of whom will settle in Toronto, Vancouver, and Montreal. Those immigrants will spend their first three months without public health care insurance. There are a further estimated 100,000 to 300,000 undocumented workers living in Canada without health-care insurance. Some come as temporary workers, or as visitors, and simply never leave. Others apply for refugee status and remain in the country even if they’re not accepted. Many have an “implied” right to be in the country because they’re applying for certain types of status, or they’re between permits. They are halfway legal, halfway not. They work, have families, buy food and clothing. They go to school, go on dates, fall in love, break up. But if they get sick, they can’t go to the hospital unless they pay up front. Or they can go without money — as long as it’s an emergency — and wait for the bill in the mail.
An accident, a sickness, or a pregnancy can leave an uninsured person with a debt they might never be able to pay off. Just one night in a hospital costs around $1,800. In intensive care it’s around $2,300 or more, depending on the treatment needed and on the hospital. For patients without much money, even a comparatively low cost — $350 up front in the emergency room, for example — can be too much. Vali remembers one man who was paying his debt to a Toronto hospital in installments of $5, every two weeks. It was all he could afford. There are a few clinics in Canada’s “big three” immigrant destination cities that see uninsured patients for free, but they are just stopgaps for a growing problem that needs a sustainable solution. The health-care community is beginning to realize it needs to make more room for these halfway people — halfway between the life they’ve left behind, yet not entirely accepted into the new one they’ve chosen.

Patients waiting for consultations in the Scarborough clinic. Photos by Arantxa Cedillo
“The problem was screaming at us,” says Caulford. In Canada, where everyone supposedly has a provincial health care card, the hospitals didn’t know what to do with people without one. Caulford had heard of many people not getting help, even in real emergencies such as broken bones, asthma, and appendicitis.
Caulford sits in a conference room at a large wooden table, donated by one of the clinic’s many supporters, with a pile of patient files in front of him. He’s volunteering here tonight and loves talking about the clinic that comes to life Tuesday and Thursday evenings, welcoming people living in Scarborough without health-care cards. The clinic opened in 2000, inspired by stories like Patricia’s. Patients arrive and sign in at the reception with Debby James, a social worker whose dark, rounded face beams with energy. When it’s their turn, the patients make their way down a narrow corridor, passing a small lounge, a washroom, three examining rooms, and a nurse’s room before arriving at the conference room, everything coated in pale-blue paint. They spend some time in the conference room speaking with D’Andrade before being guided into one of the examining rooms to wait for a doctor. A group of about 12 volunteer doctors rotate shifts to treat patients and train medical residents and foreign-trained doctors who are working to re-certify in Canada. But the clinic wasn’t always like it is today. It started with Caulford looking for doctors and Tersigni and D’Andrade for space. They recruited doctors willing to volunteer their time and found free space in a community centre and in a church basement, next to clothing boxes and decorations for the Christmas pageant. They brought medications, needles, and syringes to the sites in tackle boxes that Caulford bought at Canadian Tire. (He impressed a cashier who said, “Wow, you really like fishing! How much tackle do you have?”) At night, after seeing each patient and keeping the file for follow-up, they were often left with throat swabs, urine, and sometimes feces samples that had to be brought to the lab the next day. They would bring them home and keep them in their fridge overnight — much to the disgust of their families. Tersigni took to hiding the samples from her husband in a paper bag.
It would take Tersigni and D’Andrade about seven trips to transport all of the supplies from their cars to the MASH-type units. And because the two nurses alternated nights, they would meet sometime between Tuesday and Thursday evening to make “the switch”: they would park their cars at the side of the road and haul all of the tackle boxes and equipment from one car to the other.
They helped a lot of patients and put in long hours, but it still felt like second-rate care. “You don’t do pap smears very well in a church basement,” says Caulford. He has a friendly demeanour, and it’s easy to see how he could put even a nervous non-status immigrant at ease. He feels strongly that uninsured people should get the same level of care as everyone else, so although he was optimistic about the clinic they had put together, he worried that it wasn’t enough. “Why would it be second-rate or third-rate?”
Although the Scarborough clinic is the only clinic in Canada set up exclusively for the uninsured, there are other clinics that accept patients without coverage — but they try to keep that fact under wraps. Dr. Cécile Rousseau, a research and clinical psychiatrist at McGill University, collaborated with a team who surveyed healthcare professionals and community workers in Montreal, asking how they deal with uninsured patients. She says some clinics keep tightlipped about treating these patients because doing so is outside their mandates and they don’t want to be inundated with visits. Other clinics don’t want to draw attention for fear of their patients being targeted by immigration authorities.
Vancouver’s Bridge Clinic serves refugees and refugee claimants who get basic coverage under the Interim Federal Health Program and also has some prenatal programs for uninsured women. But it’s not enough to cover the large and growing needs of the uninsured population.
“We can’t. It’s not our mandate,” says Shirley Alvarez, the clinic’s social worker, “The clinic would be closed if we don’t follow our mandate.” Although they make some exceptions, Alvarez admits that it just scratches the surface.
“There is a need, but right now we don’t have anything to support this need,” she says.
There’s no data available in Canada that exposes the health effects of living without insurance, but research from the United States shows that a lack of insurance leads to lower-quality medical care and a higher incidence of disease. As the number of uninsured people in Canada increases, it’s getting even harder for them to access care. “There has been some tightening of the rules,” says Rousseau. “When it’s just a few people, it’s very easy to take a social and human rights approach and say, ÔOh, we’ll do it anyway.’ But when it becomes a big load on the finances of the hospital, it becomes more difficult.” She says that the first reaction has been for hospitals and clinics to close their doors to the uninsured: there are posters up in some Montreal hospitals warning people who don’t have coverage that they will have to pay. But she thinks more and more people within the health-care community are trying to work together to find solutions and to give care to everyone who needs it.
“show me where the pain is,” says Caulford to his 29-year-old patient. Alberto is standing shyly in the pale blue examining room, wearing black jeans faded in the front, a brown sweatshirt and a Budweiser baseball cap.
“It’s in my lower back. And all the way down here.” He points to his knees. “I feel, like, tingly. My legs are tingly, numb sometimes,” he says softly, with a slight Latino accent. His thin moustache and trace of a beard frame his thick lips. Caulford looks at his chart and breathes out slowly. He knows this is not just muscular pain. It’s more serious and it’s going to take a while to heal.
Alberto’s from El Salvador, the small Central American country where over a decade of civil war between guerrilla fighters and paramilitaries left a generation that grew up knowing nothing but fighting and a place where unemployed youth are often drawn into crime and violence. Alberto fled to the United States and had been living in Maryland for the last two years, working as a forklift driver in a warehouse. When an agent told him he could get a job with the same company in Toronto, where his uncle lives, he paid the agent $500 to get him across the border. He didn’t get the job. He’s been working with his uncle, who is a carpenter, but now he’s in too much pain. He doesn’t have any legal status in Canada so he’s trying to live under the radar.
“Can you stand up?” Caulford stands behind Alberto. “Just bend forward for me.”
“What? Down?” says Alberto, giving a nervous laugh and appearing embarrassed with a female resident doctor in the room. He does as the doctor says, but he can barely bend down before the pain shoots through his back.
“I think you’ve injured your disc,” Caulford tells Alberto. He draws a picture of a spine with its discs and vertebrae on the white paper sheet that covers the examining bed. He explains that there’s no magical cure for this, only medicine to take away the pain. “Avoid bending over, avoid lifting anything heavy, at least for the next three or four weeks, to let this disc heal.” He steps out to get Alberto some pain medication.
In a room across the hall, Adeola, a Nigerian woman in her 40s, is sitting with one of her legs stretched out across the examining bed. She’s wearing a brown toque and a beige-and-white-striped sweater. Her denim pant leg is rolled up and a bandage hangs open, revealing an oozing ulcer on the side of her calf. She came to the clinic for the first time last week and has just been diagnosed with diabetes. In Nigeria, Adeola was a teacher and her husband a civil engineer. Their children were all in school. They applied to Canada as landed immigrants and were accepted. “I wasn’t keen on leaving,” she says in her calm and good-humoured manner. It was her husband’s idea to emigrate.
Adeola and her family, like all permanent residents who settle in Ontario, British Columbia, Quebec, or New Brunswick, have to wait three months before getting access to public health insurance. When her ulcer first started bothering her, Adeola saw a doctor at a walkin clinic. “I had to pay for the consultation,” she says, “but he didn’t treat the wound.” She paid $100 to open a file and $30 for the consultation. But she didn’t go back, nor did she find out about her diabetes. She’s worried. Both she and her husband are having trouble finding jobs — they have no Canadian experience — and her diabetes is out of control.
The clinic is a crossroads of migrants, all arriving in different ways, but all uninsured. Unlike Alberto, who snuck into the country, Adeola and her family came as permanent residents, papers in hand. |But they’re both without public health-care insurance and have found their way to the Scarborough volunteer clinic for the uninsured. The three-month wait period for new immigrants (and for Canadians returning to the country after long stints abroad) has been in place in British Columbia for decades. In the early 1990s, Ontario and New Brunswick adopted it, with Quebec following suit at the start of the millennium. It’s supposed to prevent people from abusing our universal health-care system, but critics argue that it winds up hurting one of Canada’s most vulnerable groups. Although new immigrants are encouraged to get private insurance, they’re often not told until they arrive in the country, and at that point, many are more worried about finding a place to live, buying winter coats, and going grocery shopping than paying for private insurance, something many people didn’t have in the countries they left. Plus, private insurance doesn’t cover pre-existing conditions, so if newcomers have heart problems or diabetes, they’ll often have to pay out of pocket. Most new immigrants will be fine and won’t need any medical care for those months. Others aren’t so lucky.
Rachel Heap-Lalonde, a member of the Health Care for All Coalition in Montreal and a community worker at Project Genesis, a social justice organization, has met some of the unlucky ones. She tells of a Mexican immigrant who was hit with a debt of more than $18,000 when his 13-year-old daughter was hospitalized for appendicitis in 2003. Another couple, whose three-year-old daughter started feeling sick just days after they had arrived from Morocco, waited over a week before taking her to the hospital. The young girl ended up in intensive care with a ruptured appendix and the family was billed for over $29,000 (although the bill was later reduced to just over $18,000). In 2007, a seven-year-old boy, whose family had recently arrived from Algeria, took a nasty fall in the playground that landed him in an intensive care unit with a ruptured liver. He recovered, but his family received a $63,000 bill in the mail. Heap-Lalonde argues that huge debts can make integrating that much harder: “It might only be three months when you come, but those three months can follow you forever.”
Even the Scarborough clinic isn’t able to do much when it comes to those types of bills. Although patients referred through the clinic get a discounted price at the Scarborough Hospital, they still need to cover the cost of their hospital care. The clinic can only cover things like blood tests, throat swabs and some diagnostic tests, but if a patient needs surgery, that’s another story.
Coalitions such as Health Care for All in Montreal and Right to Health Care in Toronto are pressuring their provincial governments to do away with the three-month wait period. The governments’ response has been that the measure is necessary to avoid abuse of the system and to harmonize rules among provinces. There are some exceptions to the rules, like the decision by the Quebec government to cover care for victims of domestic abuse, sexual assault, prenatal care and deliveries, and some infectious diseases during the three-month wait period (services that are not covered automatically in the other provinces). But the ministries of health in all four provinces with the wait period say there are no plans to eliminate it any time soon.
Besides new immigrants, many temporary workers also have to wait three months for coverage. In addition, workers such as livein caregivers often go through several stints without health insurance. Because their permits are tied to the employer, if they are laid off or an elderly client passes away, they lose their work permit and have to reapply, leaving them uncovered until they get a new job and a new permit. Workers given temporary permits for less than six months — which sometimes happens in the case of live-in caregivers — are generally not eligible for public health insurance. As the number of temporary workers accepted into the country increases, the number of people with precarious insurance coverage will likely grow as well.
Refugees and refugee claimants are covered under the Interim Federal Health Program, which gives them a basic level of care. But when some claimants are denied, they stay in the country anyway, trying to keep out of sight and not get sick. Or they’ll apply to stay on “humanitarian and compassionate grounds”: that is, after the time they spent working here, they consider Canada their home and want to stay permanently. In the meantime, they’re uninsured. Others come to the country on a visitor visa and apply to be sponsored by a family member. While awaiting an answer, which can take over a year, they fall into legal limbo, in which the government knows they’re here but because they’re not really allowed, they don’t get health-care coverage. Then there are those who haven’t applied for anything; they’re just trying to get by and not make too much noise.
The fear of mammoth hospital bills, or of getting caught by immigration authorities, can dissuade people from getting help when they need it. Rousseau has heard of kids staying home with appendicitis, and of pregnant women trying to deliver their babies at home without medical help. Dr. Jacques Ramsay, a coroner in Montreal, thinks migration status has been a contributing factor in several deaths over the past few years. One Korean man, who died of a preventable heart condition, had lived in the country with his two children for less than a year. He had a visitor’s visa and had been in pain for weeks prior to his death. “He didn’t have insurance, so he didn’t go get help,” says Ramsay. When people are afraid of going to the hospital, or seeing a doctor, small problems can suddenly become fatal.
A stout, round man in a black baseball cap, red golf shirt, and jeans walks down the hall carrying a container wrapped in paper towel that’s a little wet. D’Andrade tries to introduce him to me; the man goes to put out his hand, then changes his mind and gives a nervous smile. “Steve’s got his urine with him, so go ahead, Steve!” says D’Andrade, laughing playfully.
Steve sits down in the conference room. He has a slight moustache and tanned skin. His hands are rough and weathered from years of manual labour. For eight months of every year since 1988, Steve has worked on farms in Ontario through the government’s Seasonal Agricultural Worker Program. He planted and harvested onions, carrots, celery, potatoes, lettuce, and more. “I can work from nursery to harvest,” he tells me proudly. He’s even worked on a flower farm. “I can’t remember all the names of the flowers, though,” he says with a laugh.
Back in Trinidad, Steve worked on sugar cane and rice paddies, but it wasn’t the same as working here. “Here it’s extensive mechanization. You have plots of 100 or 200 acres,” he says. “I can work all farm equipment, combines, tractors — I know it very well.” He describes working on farms with enthusiasm and says he loves Canada and has learned a lot here. So much so that in 2003 he decided to stay. His wife and sons came to meet him, but soon after, the family broke up. His wife’s sister, who lives in Toronto, helped his wife and their children apply for permanent residence status while Steve was away working on a farm. He still doesn’t have legal status here.
Steve works on the farms in the summer and in construction the rest of the year. Often he’s paid in cash, but says he uses his social insurance number whenever employers ask. “I didn’t get enough money to start an application,” he says. To apply to be a permanent resident costs more than $1,000. It also requires a lot of paperwork — not Steve’s forté.
Two years ago, he started to feel pain in his stomach and had blood in his urine. He stands up and shows me a scar down the left side of his ample belly. He had surgery last spring to take out the stones that were lodged in his kidney, blocking the urine from flowing through to the bladder. “They were rock hard,” says D’Andrade, making a fist to demonstrate. He spent five days in hospital and racked up a $4,000 bill that he’s been paying off monthly.
The wound became infected. It swelled and had to be drained of all the pus and blood that had built up. Although the clinic only ran twice a week, D’Andrade and Tersigni made sure he had it looked at every single day, often going to his apartment on the weekend to change his dressing. It finally healed in August and Steve went to work on the farm until November. He’s not eligible for disability insurance even though he’s been working here for the better part of 20 years. Now the pain on the other side of his belly is becoming unbearable and he’s scared. He doesn’t know how he’s going to survive another summer without working.
Caulford has seen a lot over the years: tuberculosis, cancer, a host of terminal diseases, and even a seven-year-old boy whose ribs had fused to his hip following a Pakistani schoolyard fight involving grenades and Molotov cocktails. You never know what you’re going to see next. But the clinic’s not a depressing place. It’s full of life, of camaraderie and selflessness. And people from all over want to share their stories, or talk about the children they’ve left in their home countries, or the ones they’ve brought to the clinic. There are colouring books and crayons. Nobody looks dangerous. No one looks “illegal.”
Among the certificates, awards, and family pictures in Caulford’s office is a painting of a boat docked in a picturesque harbour. It’s a gift, given to him by the artist, a father who immigrated to Canada a few years ago with his pregnant wife and two kids. The family had come to the uninsured clinic while under the three-month waiting period. Now he works as an accountant and his family has adapted well to life in Canada.
“You pick up the paper and you read, ÔImmigrants cause TB,'” says Caulford, annoyed at a newspaper headline. “These people enrich our lives so much — they’re not just bringing TB!” Adeola comes in for her checkup. She stops outside the reception area where James, the social worker, is sorting through the canned food on a shelf that’s available for anyone who might need it. Chunky New England Clam Chowder, Campbell’s tomato soup, and Ocean’s sockeye salmon wait in stacked cans.
“I found a job,” says Adeola quietly. She’ll be taking care of autistic children. It’s through an agency. Her husband hasn’t found anything yet, but it’s a start.
The following week, the results of Steve’s blood test came in. On top of his kidney stones ordeal, he’s just been diagnosed with diabetes.
“What’ve you been doing? Eating sugar all week?” jokes Caulford as he passes Steve and one of the nurses who are sitting in the conference room looking through a pile of flyers on diabetes. Steve smiles nervously.
In Montreal, Heap-Lalonde of the Health Care for All Coalition has gotten word that the Algerian family would no longer have to pay the $63,000 debt. It was a sigh of relief for the family after more than a year with the bill hanging over their heads — and a wave of hope for the health-care and community workers who oppose the three-month wait period. And there have been other pardons such as this one, where ministers have erased hospital debts, realizing the hardship they cause and the inability of people to pay. But just like the ad-hoc clinics across the country that help uninsured patients, the pardons are unpredictable and irregular. Meanwhile, hundreds of thousands of people living in Canada spend time without healthcare insurance, and if they get sick or have a serious accident, they could be left destitute, or worse.
If we want to keep calling our health-care system “universal,” we need to make a place for these “halfway people” and not keep giving them only half the care they need. Although he’s passionate about the clinic for the uninsured, Caulford would like to see a fundamental change. He’d like to see health-care insurance for everyone living in the country, no matter who they are or how long they’ve been here. As for the clinic, he says, “We’d love a sunset clause. We’d like to put ourselves out of business.”
Names of patients have been changed